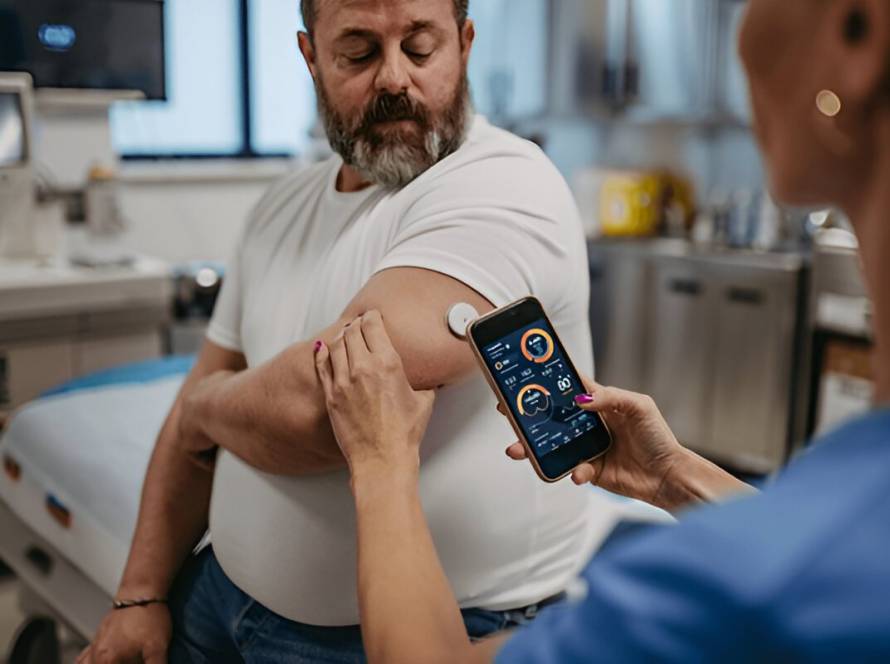
Can Remote Patient Monitoring Be the Lifeline?
Rural America is in the midst of a health care emergency and it’s been building for decades. With physician shortages, limited hospital access, and rising rates of chronic conditions, communities are grappling with a reality where health care often feels out of reach. But amidst this growing crisis, Remote Patient Monitoring in Georgia is emerging as a practical, scalable, and affordable solution to bridge the care gap.
This blog explores how RPM is not just a promising technology, but a lifeline for rural healthcare systems, clinicians, and patients across the state.

The Rural Healthcare Reality in Georgia
According to the Georgia Board of Health Care Workforce, more than 60 Georgia counties do not have a practicing OB/GYN, over 75 counties lack a paediatrician, and more than 40 counties are without a general surgeon. Combined, these Health Professional Shortage Areas (HPSAs) represent a population of just under 1.5 million Georgians struggling with access to basic healthcare services.
On top of provider shortages, seven rural hospitals in Georgia have closed since 2010, as tracked by the UNC Sheps Center for Health Services Research. For many small towns, the nearest emergency room is now over 30 miles away.
This situation has led to a crisis on multiple fronts like—logistical, financial, and clinical. When chronic conditions like hypertension, diabetes, COPD, and heart disease go unmanaged, the results are higher ER usage, preventable hospitalizations, and patient outcomes that continue to worsen.
The Case for Remote Patient Monitoring in Georgia
Remote Patient Monitoring (RPM) enables care teams to track vital signs, symptoms, medication adherence, and behavioral trends between in-person visits—delivering continuous oversight, especially for high-risk patients.
But its relevance to Georgia’s rural health crisis is even more profound.
RPM is designed for:
- Patients with limited mobility or transportation access.
- Areas with provider shortages.
- Managing chronic conditions remotely.
- Reducing avoidable readmissions and ER visits.
Studies published in Health Affairs and the Journal of Telemedicine and Telecare show that RPM can reduce readmission rates by over 40% in chronic disease populations. In Georgia, this isn’t a future promise—it’s a critical intervention.

Tackling Broadband & Technology Barriers
Some clinics hesitate, assuming RPM only works where broadband is strong. In fact, many HIPAA-compliant RPM platforms in Georgia, like localhost/kaicare/, are designed to function with cellular-based devices, requiring no Wi-Fi and minimal setup.
This makes Affordable Remote Patient Monitoring in Georgia a reality—even in counties where broadband penetration is low. According to the FCC Broadband Map and Pew Research Center, roughly 25% of rural Georgia households lack stable broadband. Cellular RPM bypasses this hurdle entirely.
Built for Chronic Care Management in Georgia
Georgia has been in the top list of states in terms of prevalence in diabetes, hypertension and cardiovascular diseases, and in particular, the rural population (CDC Rural Health Data).
As the Chronic Care Management in Georgia is currently a state and a national priority, the RPM tools allow care teams:
- Monitor the level of blood pressure, glucose, weight and oxygen on a daily basis.
- Spot warning signs before it is too late.
- Intensify adherence to medicine and tracking life goals.
This enables both patients and providers the data-driven care empowerment, and this is eligible for reimbursement with existing CMS CPT codes (CMS Fee Schedule).
Reimbursement Opportunities for Georgia Providers
A considerable number of the practices think that RPM is too costly to implement. However, CMS has introduced RPM-specific billing codes (99453, 99454, 99457, 99458) which would reimburse the practices in terms of setup, data collection, and monthly patient interaction.
Whether you’re an FQHC, primary care practice, or hospital, working with partners that offer RPM services for healthcare providers in Georgia ensures billing support and administrative guidance, so implementation doesn’t overwhelm your team.
Patient Privacy and the HIPAA Compliance
There is no compromising security. Any RPM platform of HIPAA compliance should:
- End-to-end encrypt patient data.
- Make sure that there is device-to-cloud security.
- Give clear privacy guidelines to the provider and the patient.
The privacy provisions of the federal and state levels are ensured by localhost/kaicare/ and other certified vendors.
Real Results. Real People.
RPM isn’t just a buzzword—it’s making a difference today. Georgia clinics using RPM platforms have seen:
- 30% fewer ER visits within 90 days of enrollment.
- Increased patient satisfaction scores from rural Medicaid recipients.
- Reduced staff workload complaints, made possible by automated workflows and intuitive clinical dashboards.
With the help of tailored onboarding and nurse-led monitoring teams, RPM is becoming a trusted extension of care—not a tech burden.

Conclusion:
Georgia’s rural health crisis isn’t going away. But Remote Patient Monitoring in Georgia offers a scalable, impactful, and financially viable lifeline for healthcare providers and communities.
When supported with the right tools, trained staff, and strategic platform partners, RPM has the potential to:
- Extend care without adding staff.
- Improve outcomes for chronic disease.
- Bridge the access gap for thousands of Georgians.
If you’re a rural clinic, FQHC, or provider looking to transform care delivery, now is the time to explore affordable Remote Patient Monitoring in Georgia—because the next mile in care doesn’t have to be driven. It can be delivered.
FAQs:
Q1. What is RPM and what does it mean in Rural America?
RPM is the process of monitoring patients with digital equipment that is used to measure the condition of the patient outside of a traditional clinic. RPM also fills care gaps due to provider shortages and transportation issues in rural areas of America.
Q2. Can RPM be applied to small clinics and community hospitals in America due to affordability?
Yes. Low-cost Remote Patient Monitoring has also become a reality with products, such as Kaicare, which require scalable, cost-effective, and Medicaid-compatible RPM systems and can be customized to underserved areas.
Q3. Is it HIPAA-compliant to use RPM platforms such as Kaicare?
Absolutely. RPM services provided by Kaicare will be completely HIPAA-compliant so that patient data will be secure enough but clinicians and patients can communicate without problems.
Q4. What is the positivity of RPM as far as Chronic Care Management in America is concerned?
Chronic Care Management is improved by RPM by providing a possibility to monitor the state of vitals in real-time, make timely adjustments, and engage patients more thoroughly, which all become important in the management of such conditions as hypertension, diabetes, and chronic obstructive pulmonary disease.
Q5. What has been the outcome of services offered by Kaicare RPM to healthcare providers in America?
Kaicare RPM reduces ER visits, improves patient satisfaction, and eases staff workload, extending care to rural communities.
Want to see how localhost/kaicare/ supports RPM implementation in rural Georgia? Contact us now for a live demo, reimbursement roadmap, and compliance-ready setup.